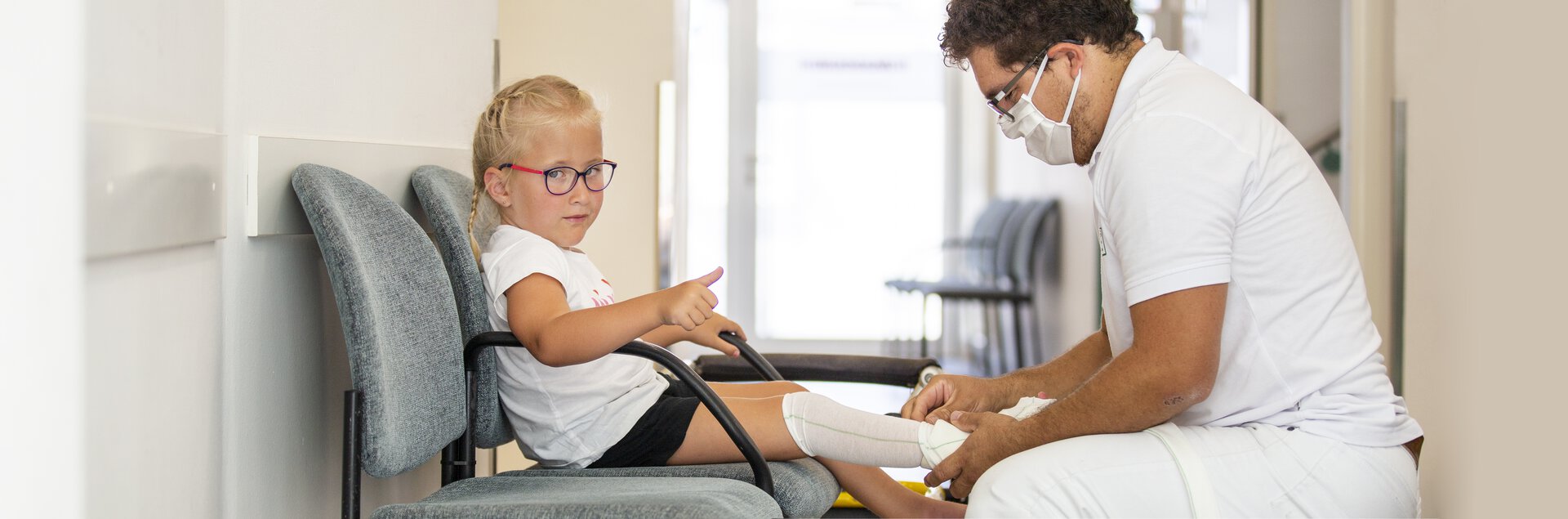
PowerHip® works using one’s own power supplied from the legs. It is developed especially for children with spina bifida (MMC).
Check out our YouTube channel for compelling stories about spina bifida patients.
Incomplete fusion of the spine
What exactly is spina bifida (myelomeningocele)?

Myelomenigocele (MMC), also known as spina bifida, is a congenital birth deformity of the spinal cord caused by failed neural tube closure during embryonic development. Symptoms of MMC vary widely.
There are two different types of spina bifida:
- Spina bifida occulta: This form of spina bifida is not noticeable from the outside. The vertebral arch is split but neither the spinal cord coverings or the spinal cord itself are affected. Since spinal bifida occulta is usually symptomless, no treatment is necessary.
- Spina bifida aperta: Spina bifida aperta is the open or visible form of spina bifida. Symptoms vary depending on how large the spinal gap is and which parts of the spinal cord are affected.
Symptoms
In two thirds of all cases, the spinal cord is damaged in the area of the lumbar spine or below. Symptoms range from increased sensitivity in the area of the lower extremities to minor impairments of walking ability and paraplegia. Disorders of bladder and bowel function can also occur.

In addition, MMC can lead to deformities of the spine and legs.
The walking ability of patients with MMC primarily depends on the level of neurological damage. Walking ability is generally not achieved in persons with affected segments of L2 or higher.
For paralysis levels between L2 and L4, walking ability is possible but usually restricted. In these cases, children rarely walk more than one hour a day and are otherwise reliant on a wheelchair for mobility. Children who have MMC affecting the lumbosacral region are usually able to walk well with the help of orthoses or insoles.
Foot deformities such as club foot and pes calcaneus are common in patients with MMC. In addition, hip contractures or hip dislocations due to muscular imbalances may also occur. Muscle imbalances can also lead to flexion or extension contractures at the knee joints. Spinal deformities such as scoliosis (estimated to affect one in two patients), fractures, and epiphysiolysis can also occur. Neurological problems resulting from Hydrocephalus have also been observed.
For children with MMC, learning to stand and walk requires extensive orthopedic and rehabilitation interventions and intensive movement therapy. On occasion, surgical operations on the feet, knee, hip and spine are required.
The Orthopedic Children’s Clinic in Aschau is one of the largest specialist clinics for pediatric orthopedics in Central Europe.
When it comes to orthopedic treatment for infants and children, it is extremely important for all parties to pull together: parents, doctors, technicians and therapists.
Physiotherapists accompany the individual treatment of our AMC patients at our headquarters and several POHLIG branches.
Start as early as possible!
Therapy
The degree of possible deformities and their effect on the neuromotor development of the child are determined by the level at which the spinal cord is damaged. If you know about the level of paralysis at an early stage, many problems can be treated preventively. Therefore, determining the extent of damage as early as possible plays a crucial role in therapy planning.
The central objective of therapy is to achieve the best possible integration of the patient into their personal and social environments. Therefore, when treating children with MMC, we attach great importance to interdisciplinary cooperation between doctors, orthopedic technicians, physiotherapists, occupational therapists and parents.


Treatment options with orthoses
Our aim is to make the best use of the child’s existing physical abilities while maximizing mobility and striving to prevent the development or progression of deformities.
For standing or walking, patients with MMC generally rely on walking orthoses that replace the non-existent muscle function. These assistive devices need to be readjusted to the patient’s height and abilities as they grow. The timing at which a walking orthosis is prescribed is based on the child’s motor development.
When considering walking orthoses, we need to take into account that the physical development of a child with MMC may be delayed compared to an unaffected child. That being said, the goal should be to have the child reach an upright posture by the time they turn three (at the latest).
Achieving an upright posture for children with MMC is considered beneficial for many reasons. Studies have shown that children who are able to be upright during their growth phase have lower rates of fractures and pressure sores. Additionally, standing allows for easier transfers and increased independence in daily life.
Briefly explained
Your questions about spina bifida
Patients with spina bifida occulta usually have an average life expectancy. In the case of spina bifida aperta, life expectancy depends strongly on the extent of the disease. If affected persons with an open back are medically well cared for, one can assume an approximately normal life expectancy. If, on the other hand, they are severely affected and have severe limitations, a lower life expectancy can be expected. However, it is not possible to make a general prediction.
To learn to stand and walk, extensive orthopedic and rehabilitation aids are often required in the case of an open back (spina bifida). This is supplemented by intensive exercise therapy and, in some cases, operations on the feet, knee and hip joints and the spine.
The causes of spina bifida have not yet been conclusively determined. An open back can be both hereditary and caused by environmental factors during pregnancy. For example, a folic acid deficiency in the expectant mother or the use of certain medications increase the risk of spina bifida.
Regardless of the trigger, one thing is certain: spina bifida develops when the neural tube does not close correctly during the 3rd-4th week of pregnancy.
Spina bifida is not curable. However, orthoses (e.g. corset, thigh orthosis, PowerHip®) and physiotherapy can counteract deformities, compensate for the restricted functions as best as possible and aim for maximum mobility of the affected person. Sometimes surgery may also be necessary to achieve an optimal treatment result.
Because spina bifida runs in families, it is suspected that genetic factors play a role. To date, however, it has not been clearly established whether spina bifida ("open back") can actually be inherited.
PowerHip® makes you mobile!
New orthosis for spina bifida patients
Many children with spina bifida are able to move around better and are more mobile overall thanks to the PowerHip® orthosis.
Weak legs
Fabian can walk with orthoses
Fabian was born with spina bifida. In the first video, the boy shows you how to put on a thigh orthosis. His orthoses replace Fabian's missing muscle function in his legs and enable him to get from A to B independently.
In the second video, you can accompany Fabian to his grandfather's farm. Equipped with various aids (crutches, orthoses, tricycle) Fabian does the farm work and explains why he would like to become a farmer when he grows up.
Canoeing with Spina bifida
Felix is thirteen years old and is soon training for the German Para Canoe national team. Since birth, the young competitive athlete has suffered from spina bifida, a spinal cord injury that makes walking difficult. That’s why Felix relies on orthoses and his wheelchair in everyday life. However, this does not prevent him from honing his technique for hours on his home river, the Main. After all, he has big goals...

Let yourself be inspired! We follow many interesting patients during their Pohlig appointment and give you personal insights.

For those who want to delve even deeper into the subject, we have a suitable video for almost every area of treatment!

Take a look behind the scenes at Pohlig and learn about different health conditions and our innovative assistive technology solutions!

Sometimes funny, sometimes explanatory, sometimes emotional - but above all always entertaining: our videos on TikTok!
All-round care!
We have the solution
Our orthopedic devices are important components of the medical and therapeutic treatment concept. Amazing results for MMC patients can be achieved in combination with physiotherapy and rehabilitation aids.
Whether you are looking for custom-made functional and positioning heels, seat shells, wheelchairs, standing and walking aids, everyday aids or orthopedic footwear – we provide you with everything you need!